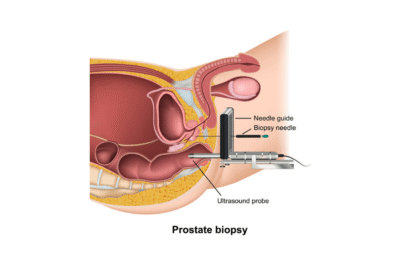
Prostate cancer remains one of the most common malignancies among men, necessitating effective and accurate diagnostic procedures. One such method gaining attention is the stabilized transperineal biopsy of the prostate. This innovative technique offers several advantages over traditional biopsy methods, making it a significant development in the field of urology.
A transperineal biopsy involves accessing the prostate through the perineum, the area between the scrotum and the anus. This approach differs from the more commonly used transrectal biopsy, which accesses the prostate via the rectum.
The term “stabilized” refers to the use of advanced imaging and mechanical stabilization techniques during the biopsy procedure. This ensures greater accuracy in targeting suspicious areas within the prostate.
The use of a stabilization device minimizes patient movement and improves the precision of needle placement, which can significantly enhance the diagnostic yield.
Reduced Infection Risk:
One of the most significant benefits of the transperineal approach is the reduced risk of severe infections and sepsis. Traditional transrectal biopsies have a higher incidence of infections due to potential exposure to rectal flora. In contrast, the transperineal route minimizes this risk.
Increased Diagnostic Accuracy:
The stabilized technique allows for better imaging guidance and needle stability, leading to improved sampling of areas suspected of harboring cancer. This can result in a higher detection rate of clinically significant prostate cancers.
Fewer Complications:
Studies suggest that transperineal biopsies are associated with fewer complications, such as bleeding and urinary retention, compared to their transrectal counterparts.
Ability to Target Multiple Areas:
The stabilization mechanism allows urologists to sample multiple areas of the prostate in a single session, which is particularly beneficial for patients with heterogeneous lesions.
Improved Patient Comfort:
With advancements in sedation and local anesthesia techniques, many patients report less discomfort during and after the procedure compared to traditional methods.
The stabilized transperineal biopsy typically involves the following steps:
Preparation:
The patient is positioned comfortably, usually lying on their back with legs in stirrups (lithotomy position). Pre-procedure imaging, such as Multiparametric MRI, is utilized to identify areas of concern.
Anaesthesia:
General or regional anaesthesia is administered as per the anaesthetist’s discretion. Local anaesthesia is also given to the perineal area to minimize discomfort in the postoperative period.
Stabilization Device Placement:
A stabilization device is applied to the perineum to ensure precise needle placement.
Biopsy:
Using Transrectal Ultrasound (TRUS) guidance, the urologist inserts a biopsy needle through the stabilized platform into the perineal area to obtain tissue samples from the prostate.
Post-Procedure Care:
After the procedure, patients are monitored for any immediate complications and given appropriate aftercare instructions.
The stabilized transperineal biopsy of the prostate represents a significant advancement in prostate cancer diagnosis. With its advantages of reduced infection risk, enhanced accuracy, and improved patient comfort, it is becoming a preferred choice for urologists and patients alike worldwide.
For men considering a prostate biopsy, discussing the transperineal option with a urologist can provide valuable insights and help make informed decisions about their health.
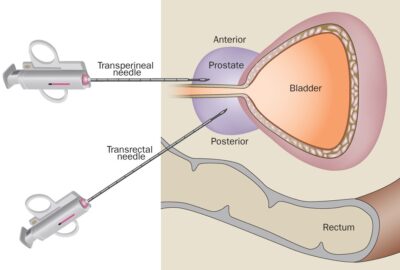
Transrectal ultrasound (TRUS) guided biopsy of the prostate is a common and minimally invasive procedure used to diagnose prostate cancer and other prostate-related conditions. This technique provides valuable information about prostate health, allowing for early detection and timely intervention.
A TRUS biopsy involves the use of ultrasound imaging to guide the collection of tissue samples from the prostate gland.
This procedure is typically recommended when a urologist suspects prostate cancer based on:
Elevated prostate-specific antigen (PSA) levels
Abnormal digital rectal examination (DRE) findings
Other risk factors associated with prostate disease
Preparation for a TRUS biopsy generally includes the following steps:
Medical Evaluation:
Your healthcare provider will review your medical history, current medications, and any previous prostate-related issues. It is important to inform them about any blood-thinning medications you are taking.
Imaging Tests:
Prior imaging, such as a Multiparametric MRI, may be performed in most cases to identify specific areas of concern within the prostate.
Antibiotics:
You may be prescribed antibiotics before the procedure to reduce the risk of infection.
Bowel Preparation:
Some providers recommend an enema before the procedure to ensure the rectum is clear.
Fasting:
If the biopsy is planned under general or regional anaesthesia, you may need to avoid eating or drinking for a few hours before the procedure.
However, if it is performed under local anaesthesia, a light breakfast is generally allowed.
Setting:
The procedure is usually performed in a clinic or hospital setting and typically takes about 20–30 minutes.
Positioning:
You will lie on your side or back, and the urologist will position a transrectal ultrasound probe in your rectum to visualize the prostate.
Anaesthesia:
Local anaesthesia may be administered to minimize discomfort. Sedation options can also be discussed with your doctor.
Biopsy Process:
The ultrasound provides real-time images of the prostate, allowing the urologist to identify areas requiring sampling. A biopsy needle is inserted through the rectal wall into the prostate to collect multiple tissue samples, ensuring accurate diagnosis.
Post-Procedure Care:
After the biopsy, you will be monitored briefly before being discharged.
It is normal to experience mild discomfort, minor bleeding, or blood in urine or semen for a few days following the procedure.
Recovery from a TRUS biopsy is generally straightforward:
Symptoms:
Mild pain, discomfort, or swelling in the rectal area, and sometimes a low-grade fever, may occur. Blood in urine or semen is also common. These symptoms typically resolve within a few days.
Activity Restrictions:
Avoid strenuous activities, heavy lifting, and sexual intercourse for a short period after the biopsy.
Follow-Up:
Your doctor will schedule a follow-up appointment to discuss biopsy results. This may take several days to a week.
While a TRUS biopsy is generally safe, there are some associated risks:
Infection:
Though rare, infections can occur and may occasionally require treatment or hospital admission.
Bleeding:
Minor bleeding is common; significant bleeding is rare.
Pain:
Discomfort during or after the procedure is expected but usually manageable.
Urine Retention:
Occasionally, post-biopsy urine retention may occur, requiring temporary catheterization.
Anxiety:
It is natural to feel anxious before or during the process. Discussing your concerns with your healthcare provider can help reduce stress and improve comfort.
A TRUS biopsy of the prostate is an essential diagnostic tool for detecting prostate conditions, especially prostate cancer.
Understanding the procedure, preparation, and recovery process can help alleviate concerns and ensure a smooth experience.
If you experience symptoms or possess risk factors related to prostate health, consult your urologist to determine whether a TRUS biopsy is appropriate for you.
Early detection is key to effective treatment and maintaining long-term prostate health.
An advanced urological test that evaluates bladder and urethral function using imaging and pressure studies. Understand how it helps diagnose urinary incontinence, bladder outlet obstruction, and neurogenic bladder with precision.
Videourodynamics (VUDS) is an advanced diagnostic test in urology that combines standard urodynamic studies with real-time imaging (fluoroscopy). It helps evaluate how the bladder, sphincter, and urethra store and release urine, providing both anatomical and functional insights.
Unlike conventional urodynamic tests, videourodynamics allows your urologist to visualize bladder function on screen while measuring pressures, giving a more accurate picture of urinary dysfunction.
This test is especially useful for diagnosing complex or unclear urinary conditions. Common indications include:
– Neurogenic bladder (due to spinal cord injury, multiple sclerosis, Parkinson’s disease)
– Bladder outlet obstruction (from prostate enlargement or urethral stricture)
– Stress or mixed urinary incontinence in women
– Post-surgical voiding dysfunction
– Unexplained urinary frequency, urgency, or retention
By combining video imaging with pressure data, the test helps differentiate between muscle-related and structural problems, guiding precise treatment plans.
The procedure is usually performed in an outpatient setting and takes about 30–45 minutes. Here’s what happens:
1. Catheter insertion: Thin catheters are placed in the bladder and rectum to measure internal pressures.
2. Bladder filling: The bladder is filled with a contrast solution visible under X-ray.
3. Monitoring: You’ll be asked to report sensations of filling, urgency, and finally to urinate.
4. Imaging: Real-time X-ray (fluoroscopy) captures the bladder and urethra during filling and emptying, while pressure sensors record the function.
The test is safe, and radiation exposure is minimal.
After the test, you may experience mild discomfort or burning during urination for a few hours. Drinking plenty of water helps flush out the contrast material and reduces irritation. Most patients resume normal activities immediately.
– Provides simultaneous visual and pressure data
– Detects subtle abnormalities missed by routine urodynamics
– Helps in accurate diagnosis of voiding dysfunctions
– Essential for treatment planning in neurogenic bladder and incontinence
– Improves surgical outcomes by identifying the exact site of obstruction or weakness
For urologists, videourodynamics is considered the gold-standard diagnostic test for evaluating lower urinary tract disorders. The detailed information it provides helps determine whether a patient needs medical therapy, behavioral modification, or surgical intervention such as bladder outlet procedures or neuromodulation.
Videourodynamics plays a vital role in understanding complex urinary issues by combining function and anatomy in one comprehensive test. It offers invaluable insights that lead to accurate diagnosis and effective, personalized treatment.
If you experience persistent urinary symptoms, consult a qualified urologist to determine whether videourodynamics can help identify the cause and guide your recovery.
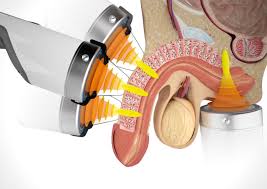
Low-Intensity Shockwave Therapy (LiSWT) is an advanced, non-invasive treatment that has revolutionized the management of erectile dysfunction (ED) and other vascular conditions affecting men’s sexual health. Unlike medications that provide only temporary relief, LiSWT addresses the root cause — poor blood flow — by stimulating natural tissue repair and regeneration.
The therapy involves delivering gentle acoustic waves (low-intensity shockwaves) to the penile tissues. These waves trigger a cascade of biological responses:
– Neovascularization: Formation of new micro blood vessels, improving penile blood flow.
– Angiogenesis stimulation: Activation of growth factors like VEGF that enhance vascular health.
– Tissue remodeling: Regeneration of smooth muscle and endothelial tissue in the corpora cavernosa.
As a result, patients often experience stronger, more sustainable erections and improved penile sensitivity over time.
– Non-invasive and painless: No anesthesia, injections, or surgery.
– Drug-free: Ideal for men who cannot tolerate PDE5 inhibitors (like sildenafil or tadalafil).
– Long-lasting results: Restores natural erectile function by promoting vascular regeneration.
– Quick sessions: Each session lasts about 15–20 minutes, with no downtime.
LiSWT is primarily used for:
– Erectile dysfunction (vasculogenic type)
– Peyronie’s disease
– Chronic pelvic pain syndrome
– Penile rehabilitation after prostate surgery
Typically, patients undergo 6 to 12 sessions over several weeks. The number of sessions may vary based on the severity of ED and individual response. Noticeable improvements in erection quality often occur within 3–6 weeks, continuing to enhance over subsequent months.
Scientific Evidence
Multiple clinical studies have demonstrated that LiSWT can significantly improve erectile function, as measured by the International Index of Erectile Function (IIEF) scores. The therapy is endorsed by leading urological associations as a promising regenerative modality, especially for men with mild to moderate ED of vascular origin.
Safety Profile
LiSWT is remarkably safe, with no reported major side effects. Patients may experience mild tingling or warmth during the procedure, which subsides quickly. Since it works by enhancing natural healing mechanisms, it offers a physiological, restorative solution rather than temporary symptom relief.
LiSWT is most effective for:
– Men with mild to moderate ED
– Those with diabetes-related vascular issues
– Patients who have partial response to oral medications
– Men seeking a natural, non-pharmacological approach
Low-Intensity Shockwave Therapy represents a breakthrough in men’s sexual health — a regenerative treatment that rejuvenates penile blood vessels, enhances natural erectile function, and restores confidence. With growing clinical support and proven efficacy, LiSWT offers a safe, effective, and lasting solution for men who wish to regain control over their sexual wellness.
Dr. Rohit Kaushal is a leading Urologist and Robotic Surgeon in Delhi, specializing in kidney transplant, prostate, and reconstructive urology with compassionate patient care.
© 2025 Created with Digital Growth Well