Advanced laser and endoscopic techniques are used to remove kidney and urinary tract stones with minimal pain and quick recovery. These minimally invasive procedures avoid large cuts, reduce hospital stays, and ensure patients return to normal life faster.
Dr. Rohit Kaushal specializes in performing safe and effective stone surgeries, including RIRS, PCNL, and URS, using the latest technology for the best outcomes.
Advanced laser and endoscopic techniques are used to remove kidney and urinary tract stones with minimal pain and quick recovery. These minimally invasive procedures avoid large cuts, reduce hospital stays, and ensure patients return to normal life faster.
Dr. Rohit Kaushal specializes in performing safe and effective stone surgeries, including RIRS, PCNL, and URS, using the latest technology for the best outcomes.
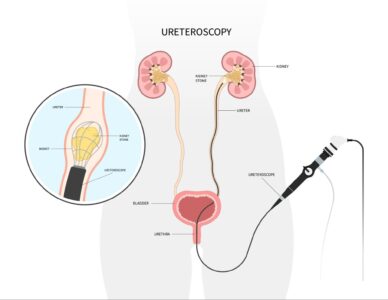
Ureteric stones, often referred to as ureteral calculi, are a common urological condition that can cause significant pain and complications. When conservative treatments fail to alleviate symptoms or resolve the obstruction, ureteroscopy emerges as a pivotal and highly effective procedure for managing these stones.
Ureteroscopy is a minimally invasive surgical procedure that allows a urologist to directly examine the ureters—the tubes that carry urine from the kidneys to the bladder. The primary purpose of this procedure, in the context of ureteric stones, is to precisely locate and then either remove or break down stones that are obstructing the urinary tract.
During the procedure, a thin, flexible or rigid tube called a ureteroscope is carefully inserted through the urethra and bladder, and then advanced into the ureter. This scope is equipped with a camera, allowing the surgeon to visualize the stones and the surrounding anatomy on a monitor. Once the stones are identified, various advanced techniques can be employed to manage them.
Ureteroscopy is typically recommended when:
Stones are too large to pass on their own (usually over 5 mm).
Stones cause significant pain, persistent urinary obstruction, or kidney swelling.
There’s an infection or an elevated risk of infection associated with the stones.
Other non-invasive treatments, such as medication or shockwave lithotripsy (ESWL), have been unsuccessful.
The ureteroscopy procedure generally involves the following steps:
Preparation: Patients may undergo pre-operative imaging studies, such as a CT scan or ultrasound, to precisely assess the size and location of the stones. Pre-operative instructions usually include fasting and adjusting certain medications.
Anesthesia: Ureteroscopy can be performed under general anesthesia or regional anesthesia (e.g., spinal block), depending on the complexity of the case and patient preference.
Insertion of Ureteroscope: The ureteroscope is carefully inserted through the urinary tract, navigating to the precise location of the stone within the ureter.
Stone Management:
Laser Lithotripsy: A tiny laser fiber is passed through the ureteroscope to deliver precise laser energy, breaking the stone into smaller fragments that can then be easily passed in the urine.
Stone Extraction: In some cases, small stones or fragments can be directly removed using specialized tools, such as graspers or stone retrieval baskets, introduced through the working channel of the ureteroscope.
Stent Placement (Optional): After the procedure, a temporary ureteral stent—a thin, hollow tube—may be placed to help drain urine, prevent swelling of the ureter, and facilitate the passage of any remaining stone fragments.
Recovery: Most patients are able to go home the same day or the next day and can typically return to normal activities within a few days.
Ureteroscopy offers several significant advantages for patients with ureteric stones:
Minimally Invasive: Unlike traditional open surgery, ureteroscopy involves no external incisions, leading to quicker recovery times, less post-operative pain, and reduced scarring.
High Success Rate: The procedure is highly effective for immediate stone removal or fragmentation, boasting a high success rate in relieving obstruction and alleviating symptoms.
Direct Visualization: The ability to directly visualize the stones in real-time allows for precise treatment, minimizing damage to surrounding tissues.
Immediate Relief: Patients often experience prompt relief from pain and obstruction once the stone is managed.
While ureteroscopy is generally considered a safe procedure, potential risks and complications can include:
Infection of the urinary tract
Bleeding
Ureteric stricture (narrowing of the ureter)
Ureteral perforation or injury
Need for additional procedures if stones are not fully removed or if complications arise
Patients should engage in a thorough discussion with their urologist to understand their specific risks and benefits prior to the procedure.
Ureteroscopy stands out as a highly effective and minimally invasive solution for managing problematic ureteric stones, providing significant relief from pain and preventing potential complications like kidney damage. With its excellent success rate and rapid recovery profile, it offers patients a practical and reliable option when conservative measures are insufficient. If you or a loved one is struggling with ureteric stones, consulting with a urologist is essential to determine the most appropriate course of action for your individual situation.
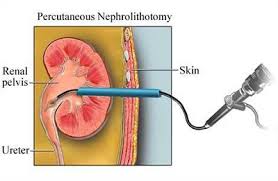
PCNL is typically recommended for patients with:
Large Kidney Stones: Generally, stones larger than 2 cm are ideal candidates for PCNL due to its high success rate in clearing significant stone burden.
Obstructive Stones: Stones causing significant blockage of the urinary tract and associated complications like infection or kidney damage.
Failed Previous Treatments: Patients who have not had success with less invasive methods such as Extracorporeal Shock Wave Lithotripsy (ESWL) or Ureteroscopy.
Complex Stones: Including staghorn calculi, which can fill a large portion of the kidney’s collecting system.
The PCNL procedure typically involves the following steps:
Anesthesia: Patients are usually placed under general anesthesia or regional anesthesia to ensure comfort throughout the procedure.
Access Creation: The surgeon creates a small incision in the back to precisely access the kidney. Guided by imaging, a dilator system creates a working channel to the kidney’s collecting system.
Nephroscope Insertion: A nephroscope (a specialized endoscope) is inserted through the created access tract to directly visualize the kidney stones.
Stone Fragmentation: Using advanced tools such as ultrasound or laser energy, the stones are carefully broken into smaller, manageable pieces.
Stone Extraction: The fragmented stone pieces are then efficiently suctioned out through the nephroscope.
Drain Placement: A nephrostomy tube may be placed temporarily to help drain urine from the kidney and ensure adequate drainage, often along with a Double J stent in the ureter.
The entire procedure usually takes about 1 to 3 hours, depending on the complexity, size, and number of stones.
Recovery after PCNL can vary by individual but generally includes:
Hospital Stay: Most patients stay in the hospital for 1 to 2 days post-surgery for monitoring and initial recovery.
Pain Management: Pain relief medications are provided to manage any post-operative discomfort.
Activity Restrictions: Patients are typically advised to avoid strenuous activities, heavy lifting, and vigorous exercise for approximately 4-6 weeks to allow for proper healing.
Follow-Up Care: Regular follow-up appointments are essential to monitor recovery, ensure complete stone clearance, and address any potential complications. The nephrostomy tube and stent are typically removed a few days or weeks after the procedure.
PCNL offers several significant advantages compared to other treatment options for large or complex kidney stones:
High Effectiveness: It is highly effective for large and complex stones, often achieving complete stone clearance in a single procedure where other methods might fail.
Minimally Invasive: With a small incision, there is less trauma to the body, resulting in less pain and a quicker recovery time compared to traditional open surgery.
Lower Risk of Recurrence: Directly removing the stones can reduce the likelihood of residual fragments and future stone formation.
Shorter Hospital Stay: Patients typically experience a shorter recovery period and hospital stay compared to more invasive open surgical approaches.
PCNL is a highly valuable and effective option for treating large and complex kidney stones. While it is generally safe and associated with excellent outcomes, it’s essential to discuss all potential risks, benefits, and alternative treatments with your healthcare provider. Early intervention and the right treatment approach can lead to better outcomes, allowing you to take control of your kidney health and lead a more comfortable life free from the pain of kidney stones.
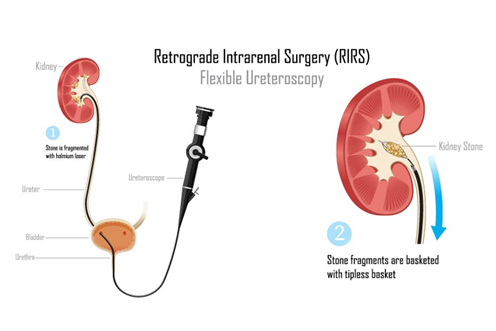
Kidney stones are a common and often painful condition affecting millions worldwide. For many patients, the search for effective treatment leads to various minimally invasive procedures. One such innovative technique is Retrograde Intrarenal Surgery (RIRS).
Retrograde Intrarenal Surgery (RIRS) is a minimally invasive procedure used to treat kidney stones, particularly those located in the renal pelvis and calyces. It involves the use of a flexible ureteroscope, which is inserted through the natural urinary tract to directly visualize and access the stones within the kidney. This advanced procedure allows for the fragmentation and removal of stones without the need for external incisions.
The RIRS procedure typically involves the following steps:
Preparation: Before the procedure, patients undergo comprehensive evaluations, including imaging studies like CT scans, to precisely determine the size and location of the stones.
Anesthesia: RIRS is usually performed under general or regional anesthesia, ensuring the patient’s comfort throughout the procedure.
Accessing the Kidney: The surgeon carefully inserts a flexible ureteroscope through the urethra, bladder, and up the ureter directly into the kidney.
Fragmentation: Once the stone is located, a laser fiber is passed through the ureteroscope to precisely break the stone into smaller pieces. These fragments can then be removed with a tiny basket or are small enough to pass naturally through the urinary tract.
Post-Procedure Care: After the surgery, a temporary ureteral stent may be placed to facilitate urine flow from the kidney and aid in the passage of any residual fragments. This stent is typically removed after a few days or weeks.
RIRS offers significant advantages for patients suffering from kidney stones:
Minimally Invasive: As it requires no incisions, RIRS leads to minimal discomfort and significantly quicker recovery times compared to traditional open surgery.
High Success Rate: RIRS has demonstrated high efficacy, especially for stones less than 2 cm in size, achieving stone-free rates comparable to other surgical methods.
Shorter Hospital Stay: Many patients can go home the same day or the day after the procedure, minimizing time away from work and daily activities.
Reduced Complications: Due to its minimally invasive nature, RIRS generally has a lower incidence of complications such as bleeding and infection compared to more invasive surgical approaches.
While RIRS is an effective treatment, it is important for patients to discuss potential risks with their urologist. These can include:
Injury to the urinary tract: Though rare, there is a small risk of injury during the insertion of instruments.
Infection: Like any surgical procedure, RIRS carries a risk of postoperative infection.
Stone Fragment Retention: Occasionally, some stone fragments may remain post-surgery, potentially requiring additional treatment.
Recovery from RIRS is generally swift. Patients are usually advised to drink plenty of fluids, manage any pain with prescribed medications, and follow up with their urologist to monitor for any complications. Straining during urination or passing small stone fragments may occur, but these symptoms typically resolve within a few days.
Retrograde Intrarenal Surgery (RIRS) is an advanced and highly effective option for treating kidney stones, particularly for those seeking a minimally invasive alternative. By understanding the procedure, its benefits, and what to expect, patients can make informed decisions about their kidney stone management. Always consult with a urologist to discuss the best treatment options tailored to individual needs.
If you’re experiencing symptoms of kidney stones or have been diagnosed with them, do not hesitate to seek medical advice. RIRS may be the solution that brings you relief and a return to a stone-free life.
Bladder stones, also known as vesical calculi or cystoliths, are hardened mineral deposits that form in the bladder. While smaller stones might pass on their own, larger or symptomatic stones often require surgical intervention. Cystolithotomy (CLT) is a traditional and effective surgical procedure used to remove bladder stones directly.
Cystolithotomy (CLT) is a surgical procedure specifically designed for the removal of bladder stones. Unlike minimally invasive endoscopic approaches, CLT involves an open surgical incision to directly access and extract the stones from the bladder. It is typically reserved for larger, more complex, or numerous bladder stones that cannot be effectively treated with less invasive methods.
CLT is often recommended in cases where:
Bladder stones are too large to be removed endoscopically.
There are multiple or recurrent stones.
Other bladder issues, such as an enlarged prostate or diverticula, need to be addressed simultaneously.
Minimally invasive options have failed or are not suitable.
The Cystolithotomy procedure generally involves the following steps:
Preparation: Before the surgery, patients undergo a thorough evaluation, which may include imaging studies such as X-rays, CT scans, or ultrasound, to confirm the presence, size, and location of the bladder stones.
Anesthesia: The procedure is performed under general anesthesia, ensuring the patient’s comfort and immobility throughout the surgery.
Incision: The surgeon makes an incision in the lower abdomen, typically just above the pubic bone, to access the bladder.
Bladder Access and Stone Removal: The bladder is then opened, and the stone(s) are directly visualized and removed. The bladder is also inspected for any underlying conditions that might contribute to stone formation, such as bladder diverticula or tumors, which may be addressed at the same time.
Closure: After ensuring all stones and fragments are removed, the bladder is carefully closed with sutures. A catheter may be left in the bladder temporarily to drain urine and promote healing. The abdominal incision is then closed.
Post-Procedure Care: Patients are monitored in recovery, and the catheter is typically removed once normal bladder function resumes.
While more invasive than some other options, CLT offers distinct advantages for specific cases:
Complete Stone Removal: Allows for the direct visualization and complete removal of even very large or multiple stones that might be difficult to access otherwise.
Addressing Underlying Issues: Enables the surgeon to address other bladder pathologies, such as bladder diverticula or prostate enlargement, during the same operation.
High Success Rate: Highly effective for definitive stone removal, often with a low recurrence rate when underlying causes are also treated.
Suitable for Complex Cases: Ideal for situations where endoscopic techniques are not feasible or have failed.
As an open surgical procedure, CLT carries certain risks that patients should discuss with their urologist:
Bleeding: As with any surgery, there is a risk of intraoperative or postoperative bleeding.
Infection: Risk of wound infection or urinary tract infection.
Pain: More significant postoperative pain compared to minimally invasive procedures.
Longer Recovery Time: Requires a longer hospital stay and recovery period.
Urinary Leakage: Though rare, temporary urine leakage from the bladder incision can occur.
Scarring: An abdominal incision will result in a visible scar.
Recovery from Cystolithotomy typically involves a hospital stay of a few days. Patients will have a urinary catheter for a period to allow the bladder to heal. Pain management, fluid intake, and activity restrictions will be advised. Follow-up appointments are essential to monitor healing, assess bladder function, and discuss strategies to prevent future stone formation.
Cystolithotomy (CLT) remains a vital and effective surgical option for patients with large, complex, or recurrent bladder stones. While it is a more invasive procedure, its ability to ensure complete stone removal and address concomitant bladder issues makes it an invaluable tool in urological practice. Patients experiencing symptoms of bladder stones should consult with a urologist to determine the most appropriate treatment plan tailored to their individual needs.
Kidney stones are a common and often painful condition that affects millions of people worldwide. While there are various treatment options available, one advanced technique gaining significant attention for its effectiveness is Endoscopic Combined IntraRenal Surgery (ECIRS).
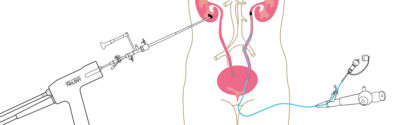
Endoscopic Combined IntraRenal Surgery (ECIRS) is a state-of-the-art, minimally invasive surgical technique used to treat kidney stones, particularly those that are large, complex, or difficult to access through traditional methods. ECIRS combines the principles of Percutaneous Nephrolithotomy (PCNL) and Retrograde Intrarenal Surgery (RIRS), allowing for comprehensive and highly effective treatment of stones located within the kidney.
The ECIRS procedure leverages a dual-access approach for optimal stone removal:
Preparation: Before the procedure, patients undergo thorough imaging studies, such as CT scans, to precisely determine the size, location, and characteristics of the kidney stones. Anesthesia is administered to ensure patient comfort during the surgery.
Accessing the Kidney (Dual Approach):
The surgeon creates a small incision in the back to insert a nephroscope (a thin, rigid tube equipped with a camera and surgical instruments). This provides direct percutaneous access to the kidney.
Simultaneously, a flexible ureteroscope is inserted through the natural urinary tract (urethra, bladder, ureter) to access the kidney from below.
Combined Techniques: By utilizing both the nephroscope and the flexible endoscope, the surgeon can simultaneously approach the stones from different angles. This dual access significantly enhances the ability to visualize, break up, and remove stones more effectively, particularly in complex anatomical situations.
Stone Fragmentation and Removal: Advanced tools, such as lasers (e.g., Holmium laser) or ultrasound devices, are used to precisely fragment the stones. The fragments are then efficiently removed through the nephroscope via suction or with retrieval instruments.
Post-Procedure Care: After the procedure, patients are monitored for recovery, and any residual stones or fragments can be managed accordingly. Most patients can expect a relatively quick recovery time.
ECIRS offers several compelling benefits for patients with kidney stones:
Minimally Invasive: ECIRS is significantly less invasive than traditional open surgery, resulting in reduced pain, minimal blood loss, and faster recovery times.
Higher Stone-Free Rates: The combined, simultaneous approach allows for more comprehensive and thorough stone removal, leading to significantly higher chances of being completely stone-free after a single procedure.
Shorter Hospital Stay: Many patients can go home within a day or two, significantly reducing the burden on healthcare resources and allowing for a quicker return to daily activities.
Less Scarring: The small incisions used in ECIRS lead to minimal scarring compared to traditional surgical methods.
Effective for Complex Cases: Particularly beneficial for large, multiple, or difficult-to-reach stones, as well as in challenging patient anatomies.
ECIRS is a versatile option suitable for patients with:
Large kidney stones (typically over 2 cm).
Stones located in challenging anatomical areas of the kidney.
Previous unsuccessful attempts at stone removal.
Complex stone burdens, such as staghorn calculi.
Patients who prefer a highly effective, minimally invasive option.
It is also considered a viable option for obese patients and those with severe cardiorespiratory compromise due to its controlled and efficient nature.
However, not all patients are ideal candidates, and a thorough evaluation by a qualified urologist is essential to determine the best treatment approach.
Recovery from ECIRS varies by individual but typically includes:
Pain Management: Patients may experience some discomfort, which can be effectively managed with prescribed medication.
Fluid Intake: Staying well-hydrated is crucial to help flush out any remaining minuscule stone fragments.
Follow-Up Appointments: Regular check-ups with the urologist are necessary to monitor recovery, ensure all stones have been effectively treated, and discuss strategies for stone prevention.
ECIRS represents a significant advancement in the management of kidney stones, combining the benefits of two powerful surgical techniques for optimal results. With its minimally invasive nature, high stone-free rates, and applicability to complex cases, ECIRS offers hope for many suffering from the pain and complications associated with kidney stones, paving the way for a smoother and more effective treatment journey. As with any medical procedure, it’s essential for patients to consult with a qualified urologist to discuss their specific conditions and personalized treatment options.
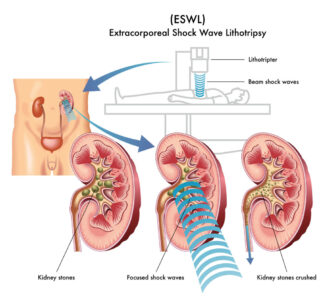
Kidney stones are a common urological issue, affecting millions of people worldwide. These small, hard mineral deposits can cause intense pain and discomfort, often leading individuals to seek effective treatment options. One of the most popular and non-invasive methods for treating kidney stones is Extracorporeal Shock Wave Lithotripsy (ESWL).
Extracorporeal Shock Wave Lithotripsy (ESWL) is a non-invasive medical procedure used to break down kidney stones into smaller fragments. The technique employs shock waves generated outside the body, which are precisely targeted at the stones, allowing them to pass more easily through the urinary tract.
The procedure begins with the patient lying on a specialized treatment table, usually in a lithotripsy machine. Here’s a step-by-step breakdown of the process:
Preparation: The patient may be given sedatives or anesthesia to ensure comfort during the procedure.
Positioning: The medical team carefully positions the patient to accurately align the kidney stones with the focus of the shock waves.
Shock Wave Generation: A series of high-energy shock waves are directed at the kidney stones. These waves are precisely guided using ultrasound or X-ray imaging to accurately locate and target the stones.
Fragmentation: The focused shock waves repeatedly hit the stones, causing them to break into smaller pieces, typically the size of grains of sand or smaller.
Natural Passage: After the procedure, these smaller stone fragments can be passed through the urinary tract naturally over the following days or weeks, often unnoticed.
ESWL is favored for several compelling reasons:
Non-Invasive: Unlike surgical options, ESWL does not require any incisions, significantly reducing recovery time and the risk of complications.
Minimal Discomfort: Most patients experience only mild discomfort during the procedure, and effective pain relief medications can be prescribed if necessary.
Outpatient Procedure: ESWL is typically performed on an outpatient basis, allowing patients to return home the same day.
High Success Rate: ESWL boasts a success rate of approximately 70-90% for stones less than 2 cm, depending on their size, location, and composition.
Quick Recovery: Most patients can return to their normal daily activities within a few days, making it a convenient treatment option.
While ESWL is generally safe, there are some important considerations and potential risks:
Stone Size and Composition: Larger stones or certain types of stones (e.g., cystine stones) may not respond as effectively to ESWL and might require alternative treatments.
Post-Procedure Discomfort: Patients may experience some mild pain or discomfort, bruising, or blood in the urine as the stone fragments pass.
Potential for Additional Treatments: In some cases, additional ESWL sessions or other procedures may be necessary if the stone fragments do not pass completely or if new stones form.
Before undergoing ESWL, patients should:
Discuss their medical history and any medications they are taking (especially blood thinners) with their healthcare provider.
Follow specific instructions regarding fasting or medication adjustments prior to the procedure.
Arrange for transportation home, as the sedation may impair the ability to drive.
ESWL is a safe, effective, and non-invasive treatment option for certain kidney stones that has transformed the way patients manage this painful condition. If you’re struggling with kidney stones, consult with your urologist to determine if ESWL is the right choice for you. With proper care and follow-up, many patients can achieve relief and return to their daily activities with minimal disruption.
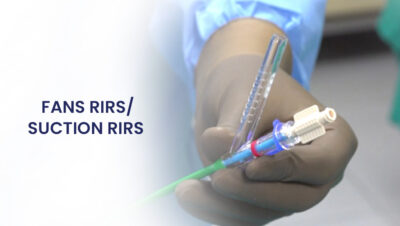
Retrograde Intrarenal Surgery (RIRS) has emerged as a gold standard minimally invasive technique for treating kidney stones and other urological conditions. Central to the success and increasing sophistication of RIRS is the innovative use of flexible and navigable sheaths. These advanced tools significantly enhance access to the renal collecting system, improve procedural efficiency, ensure complete clearance of stones and dust, and ultimately lead to superior patient outcomes.
RIRS is a sophisticated technique that utilizes a flexible ureteroscope to directly access the kidney through the natural urinary tract (urethra, bladder, ureter). Unlike traditional open surgical methods, RIRS allows for precise stone fragmentation and removal without the need for external incisions. This minimally invasive approach results in shorter recovery times and reduced postoperative discomfort for patients.
Sheaths play a crucial role in facilitating the passage and manipulation of instruments during RIRS. They act as essential conduits, allowing surgeons to navigate safely and efficiently through the ureter and into the delicate renal pelvis. The flexibility and navigability of these specialized sheaths profoundly impact the ease of access, the safety of the procedure, and the overall success of stone removal.
Modern flexible and navigable sheaths are engineered with several critical features:
Flexibility: The advanced design of these sheaths allows for precise bending and maneuvering around the complex anatomical curves of the ureter and kidney. This adaptability minimizes the risk of injury to surrounding tissues and facilitates access to challenging stone locations.
Durability: Constructed from advanced, robust materials, contemporary sheaths are both flexible and resilient, ensuring they can withstand the demands of repeated use and manipulation without compromising performance.
Optimized Lumen Size: The internal diameter (lumen) of the sheath is meticulously optimized to accommodate various essential instruments, including fine laser fibers for stone fragmentation and miniature graspers for fragment retrieval, allowing for highly effective treatment.
Ease of Insertion and Removal: Advanced design features, such as tapered tips and smooth surfaces, facilitate seamless insertion and removal, minimizing patient discomfort and improving overall procedural efficiency.
The integration of flexible and navigable sheaths significantly enhances the RIRS procedure:
Improved Access: The superior flexibility and steerability enable surgeons to access difficult-to-reach areas within the kidney’s intricate collecting system, dramatically increasing the chances of complete stone removal.
Reduced Complications: By minimizing mechanical trauma to the urinary tract during instrument passage, flexible sheaths significantly lower the risk of complications such as ureteral perforation, avulsion, or strictures.
Enhanced Visualization: Many modern sheaths are designed to optimize the flow of irrigation fluid and maintain a clear field of view, accommodating advanced imaging techniques and providing better visibility throughout the procedure.
Shorter Procedure Times: With easier navigation and consistent access, surgeons can perform RIRS more efficiently, leading to shorter operating times and reduced anesthesia exposure for patients.
Recent innovations continue to push the boundaries of sheath design and functionality:
Hydrophilic Coatings: These specialized coatings enhance the ease of insertion and navigation, reducing friction and improving overall maneuverability, especially in tortuous anatomies.
Modular Designs: Some sheaths now feature modular components that can be adjusted or replaced, offering greater versatility and adaptability for a wide range of clinical scenarios and patient anatomies.
Integration with Imaging Technologies: Advanced sheaths can now integrate seamlessly with imaging systems to provide real-time feedback, allowing for even more precise interventions and improved diagnostic capabilities.
The development and continuous refinement of flexible and navigable sheaths represent a significant advancement in the field of RIRS. By fundamentally enhancing access, minimizing complications, and improving overall procedural efficiency, these indispensable tools are transforming the landscape of urological surgery. As technology continues to evolve, we can anticipate even more innovative solutions that will further optimize patient outcomes and the effectiveness of minimally invasive procedures for kidney stones. For urologists and patients alike, embracing these advancements is key to achieving optimal care in the management of renal stones and other complex urological conditions.
Dr. Rohit Kaushal is a leading Urologist and Robotic Surgeon in Delhi, specializing in kidney transplant, prostate, and reconstructive urology with compassionate patient care.
© 2025 Created with Digital Growth Well