Minimally invasive procedures have revolutionized prostate care, offering advanced treatment for various conditions. These techniques provide precise intervention with significantly reduced recovery times. Patients benefit from less pain, fewer complications, and a faster return to daily activities. Explore the cutting-edge options available for your prostate health.
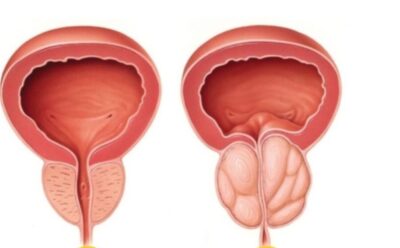
Benign Prostatic Hyperplasia (BPH) is a common condition affecting older men, characterized by an enlarged prostate gland that can obstruct urinary flow and cause various bothersome symptoms. While Transurethral Resection of the Prostate (TURP) has long been the standard surgical treatment for BPH, recent advancements have led to the development of Bipolar TURP, offering significant advantages over its monopolar counterpart.
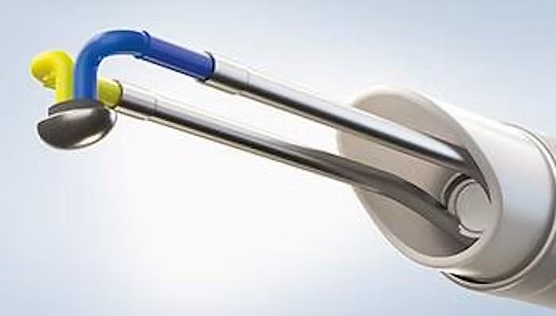
Bipolar TURP is a minimally invasive surgical procedure that uses a specialized endoscope and electrical energy to remove excess prostate tissue that is blocking urine flow. Unlike traditional monopolar TURP, which utilizes a single electrical circuit for cutting and coagulating tissue, bipolar TURP operates with two electrodes. This innovative design allows for localized energy delivery, resulting in better control over the surgical field, making the procedure safer and more effective.
Dual Electrode System: The bipolar system enables simultaneous cutting and coagulation of tissue, significantly reducing bleeding during the procedure.
Reduced Thermal Spread: Bipolar TURP minimizes thermal damage to surrounding healthy tissues, which can lead to fewer complications and a faster recovery.
Saline Irrigation: The use of a physiological saline solution instead of glycine as an irrigating fluid helps prevent complications associated with fluid absorption, such as hyponatremia (TURP syndrome).
Bipolar TURP provides several compelling benefits for patients and surgeons:
Reduced Bleeding and Transfusion Rates: One of the most significant advantages of bipolar TURP is its superior ability to control bleeding. The bipolar system’s targeted coagulation minimizes blood loss during the procedure, leading to lower rates of postoperative transfusions. This is particularly beneficial for patients who may be at higher risk for complications due to pre-existing health conditions or those on anticoagulant therapy.
Shorter Hospital Stay and Recovery Time: Patients undergoing bipolar TURP typically experience shorter hospital stays and quicker overall recoveries compared to those who have monopolar TURP. The procedure’s reduced bleeding and lower complication rates often allow patients to return to their daily activities sooner.
Lower Risk of Complications: Bipolar TURP has been associated with fewer complications, including those related to fluid overload and electrolyte imbalances. The saline irrigation greatly reduces the risk of TURP syndrome, a serious condition that can occur with monopolar TURP due to the absorption of glycine solution.
Improved Surgical Visibility: The bipolar system provides enhanced visibility of the surgical field, as the reduced thermal spread allows for better preservation of surrounding structures. This improved clarity can lead to more precise tissue removal and optimize the overall outcome of the surgery.
Enhanced Patient Safety: With reduced thermal injury and bleeding, bipolar TURP offers a safer option for patients, particularly those with larger prostates or those who need to remain on anticoagulant therapy. This added safety margin makes it a preferred choice for many urologists.
Bipolar TURP represents a significant advancement in the surgical treatment of BPH. With its advantages in terms of safety, reduced bleeding, shorter recovery times, and improved surgical outcomes, bipolar TURP has become the preferred option for many urologists and patients alike. As with any medical procedure, it’s essential for patients to discuss their specific conditions and treatment options thoroughly with their urologist to determine the best course of action for their individual needs.
Benign Prostatic Hyperplasia (BPH) is a highly common condition in aging men, characterized by an enlarged prostate that causes uncomfortable urinary symptoms. One of the latest and most significant advancements in treating symptomatic BPH is Laser Enucleation of the Prostate (LEP). This minimally invasive technique offers numerous benefits over traditional surgical options.
Laser enucleation of the prostate is a sophisticated surgical procedure designed to remove the excess prostate tissue that is obstructing urine flow. Unlike traditional methods, which may shave away tissue, LEP uses precise laser energy to target and enucleate (separate) the enlarged adenoma completely away from the prostate capsule.
The two primary types of laser enucleation utilized are:
Holmium Laser Enucleation of the Prostate (HoLEP): Utilizes a holmium laser to effectively cut, enucleate, and remove tissue.
Thulium Laser Enucleation of the Prostate (ThuLEP): Employs a thulium laser, which also provides precise tissue removal with minimal damage to surrounding structures.
LEP is widely recognized for offering superior outcomes and a gentler patient experience:
Minimally Invasive: LEP is less invasive than traditional open prostate surgery, resulting in reduced blood loss and a lower risk of complications.
Shorter Recovery Time: Patients often experience a much quicker recovery compared to traditional surgical methods, with many able to return to their normal activities within days.
Effective Symptom Relief: Clinical studies consistently show that LEP effectively and durably alleviates symptoms of BPH, including frequent urination, weak urine flow, and difficulty starting or stopping urination.
Excellent Hemostasis (Bleeding Control): For patients who must remain on blood thinners, laser enucleation proves to be an efficient therapy, offering excellent hemostasis and minimal risk of bleeding and the need for blood transfusions.
Definitive Treatment: The enucleation technique removes virtually all obstructing tissue, similar to an open prostatectomy, making recurrence of BPH symptoms highly unlikely.
During laser enucleation, the surgeon inserts a cystoscope (a thin tube with a camera) through the urethra to access the prostate. The laser is then directed at the excess prostate tissue, which is enucleated and pushed inside the urinary bladder. The removed tissues are subsequently morcellated with the help of a morcelloscope and extracted, concluding the procedure after adequate hemostasis is ensured. The surgery typically lasts about one to two hours, depending on the size of the prostate.
Recovery from LEP is generally swift. Post-procedure, patients may experience some temporary urinary symptoms, such as urgency or mild discomfort. Most are advised to:
Drink plenty of fluids to flush out the urinary system.
Avoid heavy lifting and strenuous activities for a short period.
Follow up regularly with their urologist to monitor recovery and assess urinary function.
Laser Enucleation of the Prostate represents a significant advancement in the definitive management of BPH. With its minimally invasive nature, proven long-term efficacy, and safety profile, it offers a highly promising option for many men seeking relief. As with any medical procedure, a thorough consultation with your urologist is crucial to determine the best approach tailored to your individual needs and medical history.
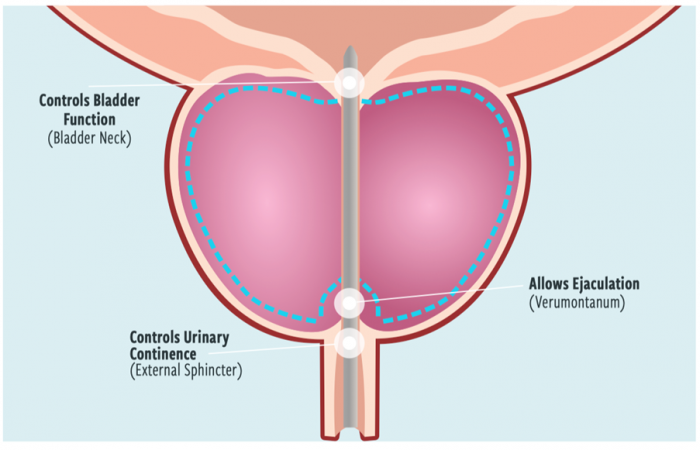
Benign Prostatic Hyperplasia (BPH), commonly known as an enlarged prostate, affects millions of men, significantly impacting their quality of life with symptoms like frequent urination, urgency, and sleep disturbances. While traditional treatment options exist, Aquablation therapy offers an innovative, minimally invasive solution.
Aquablation is a minimally invasive surgical procedure designed specifically to treat BPH. It utilizes high-velocity water jets to precisely and systematically remove obstructive prostate tissue. This technique uniquely combines the benefits of advanced robotic assistance with the gentle yet effective nature of water, providing a modern alternative to traditional prostate surgeries.
The precision and effectiveness of the Aquablation procedure stem from its reliance on advanced technology:
Preoperative Planning: Patients undergo detailed multi-dimensional imaging studies that help the urologist accurately map out the prostate’s anatomy. This meticulous planning is crucial for ensuring precise and personalized treatment boundaries.
Anesthesia: The procedure is typically performed under spinal or general anesthesia, ensuring patient comfort throughout the process.
Waterjet Technology: Using a specialized, robotic device, a high-speed, targeted water jet ablates (removes) the excess prostate tissue. The real-time imaging and robotic control allow for effective tissue removal while minimizing damage to surrounding vital areas responsible for sexual function.
Recovery: As Aquablation is minimally invasive, recovery times are generally shorter compared to traditional surgery. Patients often experience less pain and a quicker return to normal activities.
Aquablation offers several compelling benefits over conventional BPH treatments:
Minimally Invasive: The procedure requires no surgical incisions, leading to fewer complications, reduced risk of infection, and a significantly shorter recovery time.
Precision and Accuracy: The robotic assistance and real-time imaging ensure accurate and consistent tissue removal, which translates to better long-term functional outcomes and a reduced risk of side effects.
Reduced Hospital Stay: Many patients can go home the same day as the procedure or the following morning, allowing for a more convenient recovery process.
Preserved Sexual Function: Unlike some traditional surgical methods, Aquablation has demonstrated a low risk of sexual side effects, including erectile and ejaculatory dysfunction, making it a highly favorable option for many men.
Following Aquablation, patients may experience some common, temporary post-operative symptoms, which typically improve within a few days to a week:
Mild discomfort or a burning sensation during urination.
Frequent urination or urgency.
Blood in the urine (which usually resolves quickly).
Most patients can return to their regular, non-strenuous activities within a week, though heavy lifting and strenuous exercise should be avoided for a short period as advised by your urologist.
Aquablation is transforming the landscape of BPH treatment, offering a modern, highly effective, and minimally invasive option for men seeking lasting relief from their symptoms. With its unique robotic approach and promising results, it is a significant consideration for those struggling with the challenges of an enlarged prostate. It is essential to discuss your specific symptoms and medical history with your urologist to determine if Aquablation is the best fit for your individual needs.
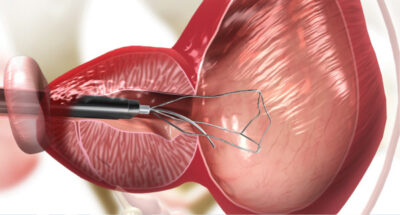
Benign Prostatic Hyperplasia (BPH) is a common condition affecting older men, characterized by an enlarged prostate that can lead to uncomfortable and disruptive urinary symptoms. While medication and traditional surgical options are available, innovative treatments like the iTIND device offer a compelling, minimally invasive alternative.
iTIND, which stands for Implantable Tension-free Urethral Device, is a novel, temporary implant designed to gently reshape the prostatic urethra and alleviate the obstructive symptoms of BPH. It is a small device inserted into the prostate through a simple, quick procedure, often performed in an outpatient setting, allowing patients to return home the same day.
The iTIND device works by applying gentle, gradual pressure to the prostatic tissue over a short period of a few days. This sustained pressure promotes the remodeling of the prostate and helps to reduce the volume of the obstructing tissue, which, in turn, alleviates lower urinary tract symptoms (LUTS) such as frequent urination, weak urine flow, and difficulty starting urination.
Insertion: The device is precisely inserted into the prostate using a cystoscope, a thin, camera-equipped tube. This procedure is typically performed under local anesthesia.
Pressure Application: Once properly positioned, the iTIND expands to exert controlled pressure on the prostate tissue, facilitating the desired anatomical changes.
Temporary Implant: The device is designed to remain in place for approximately five to seven days, after which it is easily removed, allowing the newly shaped prostatic tissue to heal and stabilize.
The iTIND device provides significant advantages over more invasive treatments:
Minimally Invasive: The procedure requires no major incisions or cutting, leading to minimal pain and a significantly quicker recovery time.
Outpatient Procedure: Patients can typically undergo the procedure and return home the same day, minimizing disruption to their daily lives.
Reduced Symptoms: Clinical studies demonstrate that patients experience significant, lasting improvements in urinary symptoms and overall quality of life following iTIND treatment.
Short Recovery: Most patients return to normal activities within days, with many experiencing relief from symptoms almost immediately after the device is removed.
Lower Risk of Side Effects: Compared to other surgical options, iTIND has a lower risk of serious complications, such as incontinence and sexual dysfunction.
Preservation of Ejaculatory Function: A critical advantage, iTIND preserves sexual and ejaculatory functions in sexually active men, a concern with many traditional BPH surgeries.
iTIND is suitable for men experiencing moderate to severe symptoms of BPH who prefer a minimally invasive treatment option. It is particularly beneficial for those who may not be responding well to medication, those who wish to avoid more invasive surgeries like prostatectomy, or patients whose underlying health makes traditional general anesthesia procedures high-risk.
The iTIND device represents an exciting advancement in the surgical treatment of BPH, offering men a less invasive and highly effective option with promising outcomes. By addressing the symptoms of an enlarged prostate safely and effectively, iTIND can significantly enhance the quality of life for many patients. Discussing the iTIND option with your urologist could be a pivotal step toward achieving lasting relief from BPH symptoms.
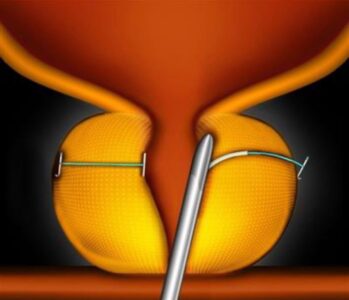
Benign Prostatic Hyperplasia (BPH) is a common and progressive condition in aging men, where the prostate gland enlarges, leading to uncomfortable and often disruptive urinary symptoms. While various treatment options exist, the UroLift® System offers a unique, minimally invasive approach to treating BPH symptoms without cutting, heating, or removing prostate tissue.
The UroLift® System is a revolutionary, minimally invasive treatment designed to relieve symptoms of BPH. It involves the insertion of tiny permanent implants that lift and hold the enlarged prostate tissue away from the urethra, thereby opening the blocked urinary passage. This procedure is typically performed in an outpatient setting, often under local anesthesia, allowing most patients to return home the same day.
The UroLift® System directly addresses the obstruction caused by an enlarged prostate:
Preparation: Prior to the procedure, a thorough evaluation, including prostate assessment, helps determine suitability for UroLift.
Anesthesia: The procedure is usually performed under local anesthesia, sometimes with light sedation, to ensure patient comfort.
Device Insertion: A slender delivery device is inserted through the urethra to reach the prostate.
Tissue Retraction: The surgeon uses the device to place small, permanent implants to pull back the encroaching prostate lobes. These implants effectively lift and hold the enlarged tissue away from the urethra, creating a wider channel for urine to flow.
Immediate Relief: Once the obstructing tissue is moved, the urethra is opened, providing immediate and significant relief from BPH symptoms.
No Tissue Removal/Heating: Crucially, the UroLift system does not involve cutting, heating, or ablating prostate tissue.
The UroLift System offers distinct advantages for men seeking relief from BPH symptoms:
Minimally Invasive: It requires no incisions, reducing the risk of bleeding, infection, and prolonged recovery typically associated with more invasive surgeries.
Rapid Symptom Relief: Many patients experience noticeable improvement in urinary flow and a reduction in symptoms relatively quickly after the procedure.
Outpatient Procedure: The treatment is generally performed in an outpatient setting, allowing patients to return home the same day and resume most normal activities quickly.
Preserves Sexual Function: A significant advantage of UroLift is that it has been clinically proven to preserve sexual function, including erectile and ejaculatory function, which is a common concern with other BPH treatments.
No Permanent Catheter: Unlike some procedures, a temporary catheter is rarely needed after UroLift, and if so, only for a very short period.
Durable Results: Clinical studies have demonstrated that the UroLift implants provide long-lasting relief from BPH symptoms.
The UroLift® System is suitable for men experiencing moderate to severe symptoms of BPH who are seeking a minimally invasive treatment option. It is particularly beneficial for those who:
Are bothered by their BPH symptoms and want to avoid daily medication.
Do not want to undergo more invasive surgical procedures.
Are concerned about preserving their sexual function.
Prefer a quick recovery with minimal downtime.
A thorough evaluation by a urologist is essential to determine if UroLift is the right treatment choice for individual needs.
The UroLift® System represents an innovative and effective advancement in the treatment of BPH. By offering a minimally invasive approach that quickly relieves symptoms while preserving sexual function, UroLift can significantly enhance the quality of life for many men. If you are experiencing symptoms of an enlarged prostate, discussing the UroLift option with your urologist could be a pivotal step toward finding lasting relief and improving your urinary health.
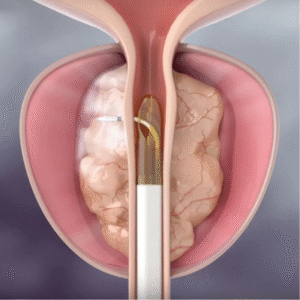
Benign Prostatic Hyperplasia (BPH) is a common condition that affects many men as they age, leading to uncomfortable and disruptive urinary symptoms. Among various treatment options, Rezūm™ Water Vapor Therapy has emerged as a groundbreaking minimally invasive solution.
Rezūm is a relatively new, highly effective treatment for BPH that utilizes the natural thermal energy of sterile water vapor (steam) to reduce excess prostate tissue. Unlike traditional surgical methods that involve cutting or ablation, Rezūm is designed to be minimally invasive, often allowing patients to return to their daily activities quickly.
The Rezūm procedure is typically performed in an outpatient setting and involves the following simple steps:
Preparation: The patient is usually given local anesthesia, sometimes with light sedation, to ensure comfort during the procedure.
Steam Delivery: A thin, flexible delivery device is inserted into the urethra and guided to the enlarged prostate tissue. The device then delivers controlled bursts of thermal water vapor directly to the targeted area.
Tissue Reduction: The steam causes the obstructive prostate cells to expand and die off (necrosis). The body naturally absorbs this treated tissue over time. This gradual process leads to a significant reduction in prostate volume, easing the pressure on the urethra and alleviating urinary symptoms.
Rezūm therapy offers distinct advantages for men seeking relief from BPH:
Minimally Invasive: Rezūm does not require any surgical incisions, significantly reducing the risk of complications and infection associated with more invasive procedures.
Quick Recovery: Many patients experience noticeable symptom relief within a few weeks and can resume normal activities shortly after the procedure.
Preservation of Sexual Function: Rezūm is clinically proven to preserve erectile function, which is a significant concern with many traditional BPH treatments.
Outpatient Treatment: The procedure is typically completed in one visit, meaning patients can go home the same day, minimizing the need for an overnight hospital stay.
Long-Lasting Results: Clinical studies have shown that the results of Rezūm therapy can last for years, providing sustained, durable relief from BPH symptoms.
Rezum is generally suitable for men with moderate to severe BPH symptoms who have not found sufficient relief through medication or who wish to avoid more invasive surgical options. A thorough evaluation by your urologist, taking into account individual health conditions and prostate anatomy, is essential to determine if Rezūm is the right treatment for your needs.
Rezum Water Vapor Therapy represents a significant advancement in the treatment of BPH, combining high effectiveness with minimal invasiveness. If you or a loved one is struggling with urinary symptoms related to an enlarged prostate, discussing the Rezūm option with your urologist could be a pivotal step toward achieving lasting relief and reclaiming your quality of life.
Prostate health is a crucial aspect of men’s wellness, particularly as they age. One of the common issues men face is Benign Prostatic Hyperplasia (BPH), which can lead to uncomfortable urinary symptoms. Among the various treatment options available, GreenLight Laser Vaporization has emerged as a leading minimally invasive procedure.
GreenLight Laser Vaporization, also known as Photoselective Vaporization of the Prostate (PVP), utilizes high-powered laser technology to precisely remove excess prostate tissue. The procedure employs a specific wavelength of light (532 nm) that is absorbed by the red blood cells. This selective absorption allows for effective tissue vaporization while simultaneously coagulating blood vessels, thus minimizing damage to surrounding structures.
The GreenLight PVP procedure follows a carefully managed process:
Preparation: Patients undergo a thorough evaluation, including medical history, physical exams, and imaging tests to accurately assess the prostate’s size and shape.
Anesthesia: The procedure is typically performed under general or regional anesthesia to ensure patient comfort throughout.
Laser Application: A cystoscope, a thin tube equipped with a camera and a laser fiber, is inserted through the urethra. The surgeon directs the laser to the obstructing prostate tissue, which is rapidly and precisely vaporized. This method effectively reduces the size of the prostate, immediately alleviating urinary symptoms.
Recovery: Most patients can expect a remarkably shorter recovery time compared to traditional surgical methods, with many able to return home the same day.
GreenLight Laser PVP offers numerous advantages over traditional surgical options:
Minimally Invasive: This technique involves no incisions, leading to significantly less pain and a quicker overall recovery.
Reduced Bleeding: The laser’s ability to coagulate vessels on contact minimizes blood loss, making it a safer option, particularly for patients who are taking blood thinners.
Immediate Symptom Relief: Many patients experience rapid and noticeable improvement in urinary symptoms, often within days of the procedure.
Shorter Catheterization: Catheterization time is usually very brief, often lasting only a day or two.
Low Risk of Complications: The procedure generally carries a lower risk of serious complications, such as long-term incontinence or erectile dysfunction, compared to more invasive surgeries.
While GreenLight Laser Vaporization is highly effective, it’s essential for patients to discuss their individual health circumstances with their urologist. Considerations include:
Prostate Size: This method is generally most effective for moderate-sized prostates. Larger prostates may require alternative surgical approaches.
Overall Health: Patients with certain pre-existing health conditions will need a detailed medical assessment to ensure suitability for this procedure.
Post-Procedure Care: Following the surgery, patients must adhere strictly to their doctor’s instructions for recovery and any advised lifestyle changes to enhance healing and long-term results.
GreenLight Laser Vaporization is transforming the way BPH is treated, offering a blend of high effectiveness and patient convenience. With its minimally invasive nature, reduced bleeding, and quick recovery time, it stands out as a modern and reliable solution for managing prostate health. As with any medical treatment, a thorough discussion with a qualified healthcare provider will help determine if this option is suitable for your specific needs.
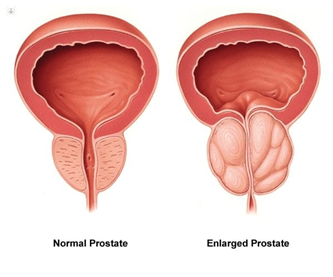
Benign Prostatic Hyperplasia (BPH) is a common condition affecting men as they age, characterized by an enlarged prostate that can lead to uncomfortable urinary symptoms. Traditional treatments often involve medication or surgical interventions, but an innovative, non-surgical procedure known as Prostate Artery Embolization (PAE) is gaining attention for its effectiveness and highly minimally invasive nature in certain groups of patients.
Prostate Artery Embolization is a minimally invasive, image-guided procedure designed to reduce the size of an enlarged prostate by selectively cutting off a portion of its blood supply. By precisely blocking the small arteries that primarily supply blood to the prostate, the procedure can induce gradual prostate tissue shrinkage over time, leading to significant improvement in urinary symptoms.
The PAE procedure is performed by an Interventional Radiologist in coordination with a Urologist, and generally involves the following steps:
Preparation: The procedure begins with a consultation and usually includes advanced imaging studies (such as CT or MRI) to precisely map out the blood supply to the prostate.
Anesthesia: PAE is typically performed under local anesthesia with light sedation, allowing the patient to remain comfortable while being awake.
Accessing the Arteries: A catheter is inserted into a small puncture in the groin or wrist and is carefully guided through the vascular system to the prostate arteries using real-time fluoroscopic imaging guidance.
Embolization: Once the catheter is correctly positioned, tiny microscopic particles (embolic agents) are injected into the arteries supplying the prostate. These particles block blood flow, effectively starving the prostate of nutrients and leading to its controlled shrinkage.
Recovery: The procedure typically lasts about one to two hours. The patient is monitored briefly, and can often return home the same day, with minimal downtime compared to traditional surgical methods.
PAE offers several compelling advantages, particularly for men seeking to avoid surgery:
Minimally Invasive: PAE does not require surgical incisions, resulting in less pain, minimal blood loss, and a much quicker recovery.
Reduced Risk of Complications: Compared to surgical options, PAE generally has a lower risk of serious complications, such as major bleeding or infection.
Shorter Hospital Stay: Most patients can return home on the same day, avoiding the prolonged recovery often associated with open or endoscopic surgery.
Preservation of Sexual Function: PAE is specifically designed to preserve erectile function and urinary continence, making it a highly appealing option for sexually active men.
Effective Symptom Relief: Clinical studies have shown that PAE can significantly improve lower urinary tract symptoms (LUTS), often providing relief comparable to more invasive procedures.
While PAE is generally safe, it is important to consider potential risks and side effects:
Infection: As with any catheter-based procedure, there is a minor risk of infection at the insertion site.
Post-Embolization Syndrome: Some patients may experience mild, temporary symptoms such as pelvic pain, urinary urgency, or flu-like symptoms after the procedure, which typically resolve within a few days.
Not Suitable for Everyone: PAE may not be appropriate for all patients, especially those with severe anatomical abnormalities or specific vascular conditions.
Prostate Artery Embolization represents a significant, non-surgical advancement in the management of BPH. As a minimally invasive alternative to traditional treatments, it offers substantial benefits in terms of recovery time, preserved function, and overall health outcomes. If you are considering options for managing your prostate health, consult with your urologist and interventional radiologist to determine if PAE is the right choice for your individual needs.
Dr. Rohit Kaushal is a leading Urologist and Robotic Surgeon in Delhi, specializing in kidney transplant, prostate, and reconstructive urology with compassionate patient care.
© 2025 Created with Digital Growth Well