Robotic Urology Surgery is an advanced, minimally invasive surgical technique that uses robotic-assisted technology for greater precision, control, and faster recovery. It allows surgeons to perform complex urological procedures through small incisions with the help of high-definition 3D visualization and robotic arms that mimic human hand movements.
Under the expert guidance of Dr. Rohit Kaushal, this cutting-edge technology is used to treat conditions related to the prostate, kidneys, and bladder, including cancers and obstructions. The approach ensures less pain, minimal blood loss, shorter hospital stays, and faster return to normal activities compared to traditional open surgeries.

The field of surgery has been dramatically transformed over the past few decades by technological advancements. One of the most exciting developments is the advent of robot-assisted surgery. Among the many benefits it offers, robot-assisted partial nephrectomy stands out as a testament to how innovation can enhance surgical precision, reduce patient recovery time, and improve outcomes.
Partial nephrectomy is a surgical procedure aimed at removing a portion of the kidney, typically due to the presence of a tumor or localized renal cell carcinoma. The primary goal is to excise the diseased part of the kidney while preserving as much of the healthy tissue as possible. Traditional approaches to this surgery include open surgery and laparoscopic surgery. However, the advent of robotic technology has introduced a new, more refined technique: robot-assisted partial nephrectomy.
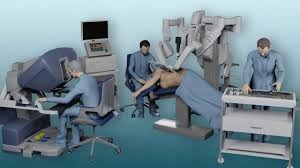
Robot-assisted surgery utilizes advanced robotic systems, such as the da Vinci Surgical System, which allows surgeons to perform intricate and delicate procedures with unprecedented precision. The system consists of a console where the surgeon sits and controls robotic arms equipped with specialized surgical instruments. High-definition, 3D visualization provides a magnified view of the surgical site, ensuring meticulous movements and enhanced accuracy.
Robot-assisted partial nephrectomy offers numerous benefits for patients:
Enhanced Precision and Control: Robotic systems translate the surgeon’s hand movements into smaller, more precise actions of the surgical instruments. This level of control is particularly important in kidney surgery, where sparing as much healthy tissue as possible is crucial for preserving kidney function.
Minimally Invasive: Incisions made during robot-assisted surgery are significantly smaller compared to traditional open surgery. This minimally invasive approach results in less postoperative pain, reduced scarring, and shorter hospital stays.
Reduced Blood Loss: Robotic precision helps minimize blood loss during the surgery, lowering the risk of complications and the potential need for blood transfusions.
Faster Recovery: Patients typically experience faster recovery times with robot-assisted partial nephrectomy. The minimized trauma to the body means patients can return to their normal activities sooner.
Better Functional Outcomes: Studies have shown that robot-assisted partial nephrectomy offers excellent oncological outcomes while preserving kidney function more effectively than traditional methods.
Preoperative Preparation: Before the surgery, patients undergo comprehensive evaluations, including advanced imaging studies such as CT scans or MRIs to pinpoint the exact location and size of the tumor. Blood tests and other assessments ensure the patient is ready and healthy for surgery.
Surgical Procedure: Under general anesthesia, the patient is positioned, and small incisions are made in the abdomen to insert the robotic instruments. The surgeon sits at the console, controlling the robotic arms to perform the procedure. The diseased part of the kidney is carefully removed, and the remaining healthy tissue is meticulously sutured.
Postoperative Care: After the procedure, patients are monitored in the recovery room before being moved to a hospital room. Most patients are discharged within a few days. Follow-up appointments are crucial to ensure proper healing and assess long-term kidney function.
Robot-assisted partial nephrectomy represents a significant leap forward in the field of kidney surgery. With its numerous benefits, including enhanced precision, minimally invasive techniques, reduced recovery time, and excellent functional outcomes, it offers a promising option for patients facing kidney tumors. As technological advancements continue to evolve, the landscape of surgery will undoubtedly keep shifting towards more efficient and less invasive techniques, contributing to improved patient care and quality of life. If you are a candidate for partial nephrectomy, discussing the possibility of robot-assisted surgery with your healthcare provider might open doors to a smoother, more precise surgical experience.
The diagnosis of cancer is a profound and often overwhelming experience. However, continuous advancements in modern medical technology are transforming treatment landscapes, offering more effective and less invasive methods that significantly improve patient outcomes and quality of life. Among these groundbreaking procedures is the Robot-Assisted Radical Cystectomy (RARC).
A radical cystectomy is a comprehensive surgical procedure involving the removal of the entire bladder and often some of its surrounding organs and tissues, primarily to treat bladder cancer. For men, this typically includes the removal of the prostate and seminal vesicles. For women, it may involve the removal of the uterus, ovaries, and a portion of the vaginal wall. While a complex and extensive procedure, it is frequently a necessary intervention to prevent the further spread of cancer.
Robot-Assisted Radical Cystectomy elevates the traditional radical cystectomy by integrating advanced robotic technology. This sophisticated system provides surgeons with enhanced dexterity, unparalleled precision, and superior control. Essentially, the robotic arms function as an extension of the surgeon’s hands, enabling the execution of highly intricate procedures through only a few tiny incisions.
RARC offers numerous advantages compared to traditional open surgery:
Minimally Invasive: As a minimally invasive procedure, RARC involves smaller incisions, leading to significantly less blood loss, reduced post-operative pain, and a lower risk of complications such as infections.
Faster Recovery: The less invasive nature of RARC generally translates to a quicker recovery period for patients. This includes shorter hospital stays, a faster return to normal daily activities, and overall better postoperative outcomes.
Improved Precision: The robotic system empowers the surgeon to operate with heightened precision. This is particularly critical in the delicate pelvic area, which contains numerous vital structures like nerves, blood vessels, and organs. Enhanced precision facilitates more accurate excision of cancerous tissues while maximizing the preservation of healthy tissue.
Reduced Pain and Scarring: Due to the smaller incisions made during RARC, patients typically experience less postoperative pain and scarring, contributing to a more comfortable recovery experience.
Better Visualization: The robotic platform delivers a high-definition, 3D view of the surgical site. This magnified and illuminated perspective provides surgeons with a superior understanding of the surgical field compared to what the naked eye can offer, thereby improving their ability to make precise incisions and sutures.
During a Robot-Assisted Radical Cystectomy, the patient is under general anesthesia. The surgeon controls the robotic arms from a nearby console, manipulating tiny surgical instruments such as scissors, scalpels, and forceps attached to these arms.
The procedure typically involves the following steps:
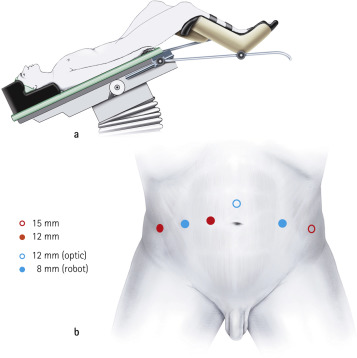
Preparation and Incisions: Small incisions are made in the abdomen through which the robotic instruments and a high-definition camera are inserted.
Removal of Bladder and Tissues: The surgeon meticulously removes the bladder and any surrounding tissues or organs as dictated by the extent of the cancer.
Urinary Diversion: A crucial step involves creating a new pathway or reservoir for urine storage and passage. This can be achieved through several methods, including an ileal conduit, continent cutaneous diversion, or orthotopic neobladder reconstruction.
Closure: The small incisions are carefully closed, often with absorbable sutures. Post-surgery, blood thinner injections are typically prescribed for approximately one month to mitigate the risk of deep vein thrombosis.
Robot-Assisted Radical Cystectomy represents a significant leap forward in the treatment of bladder cancer, seamlessly integrating surgical expertise with cutting-edge technology. Its minimally invasive nature bestows numerous benefits upon patients, ranging from reduced postoperative pain to accelerated recoveries. As RARC continues to gain widespread acceptance and refinement, it holds immense promise for improving outcomes not only for bladder cancer patients but potentially for a broader spectrum of complex surgical procedures.
The field of medicine is continuously evolving, with the integration of robotics into surgical procedures marking one of the most exciting advancements. Among these innovative techniques, Robot-Assisted Radical Prostatectomy (RARP) stands out as a transformative solution in the treatment of prostate cancer.
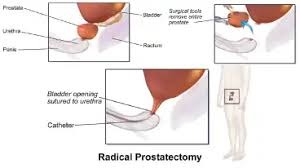
Robotic radical prostatectomy is a minimally invasive surgical procedure utilized to remove the prostate gland in patients diagnosed with prostate cancer. This procedure is performed using advanced robotic systems, such as the da Vinci Surgical System or other newer platforms, which empower surgeons to operate with enhanced precision, flexibility, and control. The robotic system translates the surgeon’s hand movements into smaller, highly exact movements of tiny instruments inside the patient’s body.
The RARP procedure follows a carefully orchestrated sequence:
Preparation: The procedure begins with the patient being sedated under general anesthesia. Small incisions, rather than one large one, are made in the patient’s abdomen.
Robotic Assistance: The surgeon sits at a console near the patient and operates the robotic arms. These arms are equipped with a high-definition camera and specialized surgical instruments. The console provides the surgeon with an immersive, 3D view of the surgical site.
Precision Surgery: The robotic system translates the surgeon’s hand movements into precise micro-movements of the surgical instruments, allowing for meticulous dissection and removal of the prostate gland and any necessary surrounding tissues.
Completion: Once the prostate and associated tissues are removed, the incisions are carefully closed, and the patient is transferred to the recovery area.
Robotic radical prostatectomy offers several significant advantages over traditional open surgery and even conventional laparoscopic techniques:
Minimally Invasive: Smaller incisions result in less trauma to the body, significantly reduced bleeding, and minimized scarring.
Enhanced Precision: Robotic systems provide surgeons with unprecedented control and dexterity, facilitating nerve-sparing techniques that can help preserve crucial urinary and sexual function.
Reduced Pain and Recovery Time: Patients often experience less postoperative pain and benefit from quicker recovery times compared to open surgery, allowing for a faster return to normal activities.
Fewer Complications: The superior precision of robotic surgery often translates to fewer complications, such as infections and significant blood loss.
Improved Cancer Control: Studies have indicated that robotic surgery can result in lower positive surgical margins, meaning a reduced likelihood of cancer cells being left behind after removal.
Understanding the patient journey is key to a successful outcome:
Before Surgery: Patients will undergo a thorough evaluation and consultation with their medical team to determine their eligibility for robotic radical prostatectomy. Preoperative tests, including blood work and imaging, are typically required. Patients will also receive detailed instructions on preparing for surgery, such as fasting and medication adjustments.
During Surgery: The procedure can take several hours, but patients will be under general anesthesia and will not feel anything during the operation. The surgical team will closely monitor the patient’s vital signs throughout the procedure.
After Surgery: Recovery typically involves a hospital stay of one to two days. Patients may have a catheter in place to drain urine for a short period post-surgery. Mild pain and discomfort at the incision sites are common but can be effectively managed with prescribed medications. Blood thinner injections are prescribed for about a month after surgery to decrease the risk of deep vein thrombosis.
Long-term Recovery: Patients will gradually resume normal activities within weeks. Follow-up appointments will be scheduled to monitor recovery and address any concerns. It’s important for patients to openly discuss potential side effects, such as changes in urinary or sexual function, with their doctor. Rehabilitation exercises and therapies may be recommended to aid in a comprehensive recovery.
Robotic radical prostatectomy represents a significant advancement in the treatment of prostate cancer, offering patients a less invasive option with numerous benefits. If diagnosed with prostate cancer, discussing robotic surgery with your urologist can provide valuable insights into the most appropriate and tailored treatment plan for your individual needs.
In the realm of urology, innovative surgical techniques are continually evolving to enhance patient outcomes and minimize recovery times. One such technique gaining significant attention is robotic-assisted Boari flap reconstruction. This advanced procedure offers new hope for patients facing complex urinary tract reconstruction challenges.
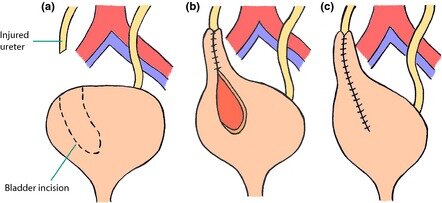
The Boari flap is a well-established surgical technique primarily used for reconstructing the urinary tract when there is an irreversible obstruction or damage in a portion of the ureter. Traditionally, this procedure involves mobilizing a portion of the bladder to create a flap that connects the bladder to the ureter, effectively bypassing any obstructed or damaged segments.
It is commonly indicated in cases of:
Ureteral strictures
Bladder tumors
Complications following radical pelvic surgery
Robotic surgery has transformed many fields of medicine, including urology. With the introduction of robotic systems like the da Vinci Surgical System, surgeons can perform complex procedures with enhanced precision, reduced blood loss, and shorter recovery times.
The key benefits of robotic surgery include:
Improved Visualization: 3D high-definition views allow surgeons to navigate intricate anatomical structures with superior clarity.
Enhanced Dexterity: Robotic instruments provide a greater range of motion and articulation compared to traditional laparoscopic tools, enabling more intricate and precise maneuvers.
Minimally Invasive Approach: Smaller incisions lead to less postoperative pain, shorter hospital stays, and a quicker return to daily activities
Robotic Boari flap reconstruction is indicated for various conditions, including:
Ureteral strictures (narrowing of the ureter)
Bladder cancer with subsequent reconstruction needs
Congenital anomalies affecting urinary tract anatomy
Complications from previous surgeries in the pelvic region
Robotic Boari flap reconstruction represents a significant advancement in the field of urological surgery. By seamlessly combining the established effectiveness of the Boari flap technique with the unparalleled precision and minimally invasive nature of robotic surgery, patients can experience better outcomes with fewer complications and faster recoveries.
As technology continues to evolve, the future of urological surgery looks promising, providing hope and improved quality of life for many patients facing complex urinary tract challenges. If you or a loved one is facing urinary tract issues, consult a qualified urologist to discuss the potential benefits of robotic-assisted surgeries, including Boari flap reconstruction. With the right approach, recovery can be both swift and successful.
In recent years, advancements in technology have significantly transformed the field of medicine. One of the most notable innovations is the use of robotic systems in surgical procedures, particularly in kidney transplantation. This exploration delves into the evolution, benefits, challenges, and future of robotic kidney transplants.
Robotic kidney transplantation involves utilizing robotic-assisted surgical systems to perform kidney transplants. Unlike traditional open surgeries, which necessitate large incisions and longer recovery times, robotic procedures employ smaller incisions and advanced imaging. This approach provides surgeons with enhanced precision and control, leading to a less invasive procedure for the patient.
Robotic surgery is not a brand-new concept. The first robotic-assisted surgical procedure was performed in the late 1980s, but it wasn’t until the early 2000s that robotic systems gained widespread acceptance in urology and organ transplantation. The da Vinci Surgical System is one of the most widely used robotic platforms, empowering surgeons to perform intricate tasks with greater dexterity and a magnified, 3D view of the surgical field.
The adoption of robotic technology in kidney transplantation offers several compelling advantages:
Minimally Invasive Approach: One of the primary advantages is its minimally invasive nature. Smaller incisions result in less trauma to the body, leading to reduced pain and quicker recovery times for patients. Most patients can leave the hospital within a few days, a significant improvement compared to longer stays associated with traditional open surgery.
Enhanced Precision: Robotic systems provide surgeons with a high-definition 3D view of the surgical site and allow for precise, tremor-free movements. This enhanced precision is particularly crucial in delicate procedures like kidney transplantation, where accurate placement and connection of the new organ are vital for optimal function and to minimize complications.
Reduced Complications: Studies have indicated that robotic kidney transplants can lead to fewer complications compared to traditional methods. This includes lower rates of infection, less blood loss, and a decreased need for blood transfusions.
Improved Outcomes: Patients undergoing robotic kidney transplants often experience better functional outcomes, including improved kidney function and shorter hospital stays. The minimally invasive nature of the procedure can lead to quicker recovery times, allowing patients to return to their daily activities sooner and with less discomfort.
Despite the many advantages, robotic kidney transplantation is not without its challenges:
Cost: Robotic surgical systems represent a substantial investment in terms of purchase and ongoing maintenance. This can contribute to higher costs for patients and healthcare systems. Insurance coverage can vary, and not all hospitals are equipped with the latest robotic technology.
Surgeon Training: Performing robotic surgery requires specialized, extensive training and a significant learning curve. Surgeons must become proficient in utilizing these complex robotic systems, which can demand considerable time and resources. Consequently, not all transplant centers have immediate access to surgeons with this specialized expertise.
Limited Availability: Not all medical facilities currently offer robotic kidney transplantation. Patients may, therefore, need to travel to specialized centers, which can be inconvenient and incur additional costs.
As technology continues to evolve, the future of robotic kidney transplantation looks exceptionally promising. Research is ongoing to improve robotic systems, making them more accessible and cost-effective. Innovations such as artificial intelligence (AI) and enhanced imaging techniques may further refine the precision and efficiency of these procedures, potentially leading to even better patient outcomes.
Additionally, as the demand for organ transplants continues to grow globally, robotic surgery may play an increasingly critical role in addressing the shortage of available organs. By improving surgical outcomes, expanding the pool of suitable candidates, and potentially broadening access, robotic kidney transplantation holds the potential to significantly impact patient care and redefine the landscape of transplant medicine.
Robotic kidney transplantation represents a significant leap forward in surgical techniques, offering numerous benefits over traditional methods. While challenges related to cost, training, and availability remain, ongoing advancements in technology and specialized training promise to enhance this field further. As we look to the future, robotic surgery holds the profound potential to redefine kidney transplantation and improve the lives of countless patients worldwide.
Robotic pyeloplasty is a cutting-edge, minimally invasive surgical procedure designed to correct ureteropelvic junction obstruction (UPJO). This condition, if left untreated, can lead to significant kidney damage. This innovative technique seamlessly blends advanced robotic technology with established surgical principles to enhance precision, reduce recovery times, and ultimately improve patient outcomes.
Ureteropelvic junction obstruction occurs when there is a blockage at the critical junction where the ureter (the tube carrying urine from the kidney to the bladder) meets the kidney. This obstruction can lead to a range of issues, including:
Swelling of the kidney (hydronephrosis)
Flank pain
Hematuria (blood in the urine)
Recurrent urinary tract infections (UTIs)
Potentially irreversible kidney damage
The obstruction can be congenital, present from birth due to abnormalities during fetal development, or acquired later in life due to factors such as:
Kidney stones
Tumors
Scar tissue from previous surgeries
Diagnosis typically involves advanced imaging studies such as ultrasounds, CT scans, and DTPA scans, which are crucial for assessing kidney function and determining the severity of the obstruction.
Robotic pyeloplasty utilizes sophisticated robotic surgical systems, such as the da Vinci Surgical System, to facilitate the surgery. The procedure generally follows these meticulous steps:
Preparation and Anesthesia: The patient is placed under general anesthesia and carefully positioned to ensure optimal surgical access.
Trocar Placement: Several small incisions are made in the abdomen to insert trocars (hollow tubes). These serve as precise entry points for the robotic instruments and a high-definition 3D camera.
Robot-Assisted Dissection: The surgeon operates from a console, manipulating the robotic instruments with unparalleled dexterity. The console provides a magnified, high-definition 3D view of the surgical field, allowing for exceptionally precise dissection around the obstructed area.
Reconstruction: Once the obstructed segment is meticulously removed, the surgeon reconstructs the ureter to ensure proper and unobstructed drainage from the kidney. At the conclusion of the procedure, a Double J stent is placed across the anastomosis (the newly joined section) to support healing and is typically removed after a few weeks. A surgical drain may also be placed for a day or two around the surgical site to remove any fluid or blood collection, which is subsequently removed.
Closure: The small incisions are meticulously closed with sutures, and the patient is closely monitored during the initial recovery phase.
Robotic pyeloplasty offers significant advantages over traditional open surgical methods:
Minimally Invasive: Smaller incisions lead to considerably less postoperative pain and significantly faster recovery times.
Enhanced Precision: The robotic system provides greater dexterity, range of motion, and a stable, magnified 3D view, allowing for incredibly precise surgical maneuvers and minimizing damage to surrounding delicate tissues.
Reduced Blood Loss: The precision of the robotic technique often results in lower intraoperative blood loss, thereby decreasing the need for blood transfusions.
Shorter Hospital Stay: Many patients can be discharged within 24 to 48 hours post-surgery, facilitating a quicker return to normal daily activities.
Improved Outcomes: Studies consistently demonstrate that robotic pyeloplasty achieves similar or even improved success rates compared to open surgery, often with lower complication rates.
Following surgery, patients are typically monitored for a short period before being discharged. Emphasis is placed on effective pain management, adequate hydration, and a gradual return to normal activities. Follow-up appointments are crucial and usually involve repeat imaging studies and urine tests to confirm the complete resolution of the obstruction and ensure normal kidney function.
Robotic pyeloplasty represents a significant advancement in the effective treatment of ureteropelvic junction obstruction. By leveraging the immense benefits of robotic technology, surgeons can offer patients a safer, more effective surgical option that promotes quicker recovery and superior overall outcomes. As medical technology continues to evolve, we can anticipate further enhancements in surgical techniques that will continue to improve patient care and revolutionize urological procedures.
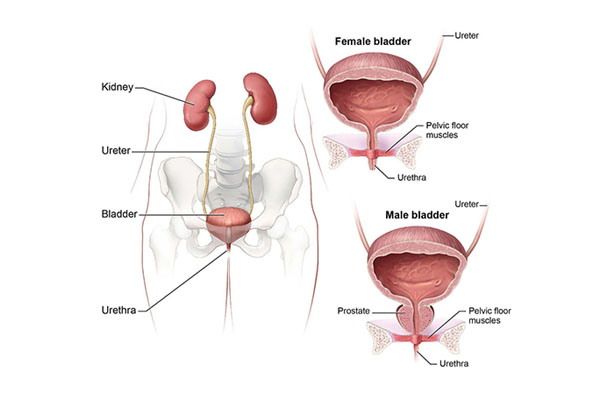
Ureteric reimplantation is a crucial surgical procedure designed to correct conditions such as vesicoureteral reflux (VUR) or ureteral obstruction. Traditionally performed through open surgery, significant advancements in medical technology have led to the emergence of highly effective robotic-assisted techniques.
Robotic ureteric reimplantation utilizes sophisticated robotic surgical systems, such as the da Vinci Surgical System, to assist surgeons in performing the reimplantation with enhanced precision and control. This system facilitates minimally invasive techniques, which can lead to superior patient outcomes and significantly quicker recovery times.
The integration of robotic technology into ureteric reimplantation offers numerous advantages for patients:
Minimally Invasive: Robotic surgery involves smaller incisions compared to traditional open surgery, resulting in less tissue trauma, reduced postoperative pain, and improved cosmetic results.
Enhanced Precision: The robotic system provides surgeons with high-definition 3D visualization and unparalleled dexterity, enabling them to navigate complex anatomical structures with greater ease and accuracy.
Faster Recovery: Patients typically experience shorter hospital stays and a quicker return to normal daily activities due to the reduced surgical trauma associated with minimally invasive approaches.
Lower Complication Rates: Studies indicate that robotic techniques may lead to fewer complications, such as infections or urinary tract issues, enhancing overall patient safety.
The process for robotic ureteric reimplantation involves several key steps:
Preoperative Preparation: Patients undergo a thorough evaluation, including advanced imaging studies (such as CT scans or MRIs) and potentially a urodynamics test, to comprehensively assess the condition of the urinary system.
Anesthesia: The procedure is performed under general anesthesia to ensure patient comfort and immobility.
Surgical Technique: The surgeon makes several small incisions in the abdomen. Robotic arms, equipped with specialized surgical instruments and a high-definition camera, are then carefully inserted. From a console, the surgeon skillfully operates the robotic system, utilizing the 3D visualization to precisely reimplant the ureter into the bladder.
Closure: Upon successful completion of the reimplantation, the small incisions are meticulously closed, often with absorbable sutures.
Recovery from robotic ureteric reimplantation is generally swift and less demanding than traditional open surgery. Patients can typically expect:
Hospital Stay: Typically 1 to 2 days, depending on individual recovery progress.
Pain Management: Postoperative pain is usually minimal and can be effectively managed with standard medications.
Follow-Up: Regular follow-up appointments are essential to monitor recovery, assess kidney and bladder function, and ensure optimal long-term results.
Robotic ureteric reimplantation represents a significant advancement in urological surgery, offering numerous benefits over traditional methods. With its minimally invasive nature and enhanced precision, patients can anticipate better clinical outcomes and a quicker return to their normal lives. If you or a loved one is facing ureteral issues, consulting with a qualified urologist is a vital step to explore the possibility of robotic surgery as a cutting-edge treatment option.
Penile cancer, though relatively rare, presents significant challenges for both patients and healthcare providers. Traditional treatment options often involve radical surgery, which can lead to extensive physical and emotional repercussions. However, advancements in medical technology have paved the way for less invasive procedures, such as Robotic VEIL (Video-Endoscopic Inguinal Lymphadenectomy) surgery.
VEIL surgery is a minimally invasive technique specifically designed to address lymph node involvement in penile cancer. The procedure utilizes robotic assistance to enhance precision and control during surgery, ultimately leading to improved outcomes for patients.
Robotic surgery employs advanced robotic systems that allow surgeons to perform delicate operations with enhanced visualization and dexterity. The robot’s articulated instruments provide a greater range of motion than the human hand, making it ideal for complex surgeries like VEIL. The procedure is typically performed through small incisions, which means less trauma to the body compared to traditional open surgery.
Robotic VEIL surgery offers numerous advantages for patients:
Minimally Invasive: The small incisions used in robotic VEIL surgery lead to reduced blood loss and a lower risk of infection. Patients often experience less postoperative pain and a quicker recovery.
Enhanced Precision: The robotic system provides superior 3D visualization, allowing surgeons to navigate the intricate anatomy of the groin region with greater accuracy. This precision is crucial for successful lymph node dissection.
Shorter Hospital Stay: Many patients undergoing robotic VEIL surgery can expect to go home the same day or the following day, as the procedure is less invasive and promotes faster recovery times.
Better Aesthetic Outcomes: With smaller incisions, patients benefit from reduced scarring, which can be an important consideration for those concerned about body image post-surgery.
Improved Functional Outcomes: Studies suggest that robotic VEIL may preserve nerve function better than traditional approaches, potentially leading to improved sexual function and overall quality of life for patients.
Robotic VEIL surgery typically involves the following steps:
Preparation: Before the procedure, patients undergo thorough evaluations, including imaging studies and cancer staging. This helps the surgical team develop a tailored approach.
Anesthesia: The patient is placed under general anesthesia for comfort during the surgery.
Incision and Port Placement: Small incisions are made in the abdomen and groin. The robotic arms are inserted through these ports.
Lymph Node Dissection: The surgeon uses the robotic system to carefully dissect and remove lymph nodes in the groin, assessing for any signs of cancer spread.
Closure: Once the procedure is complete, the small incisions are closed with sutures, and the patient is monitored in recovery.
Robotic VEIL surgery is typically recommended for patients with localized penile cancer who have evidence of lymph node involvement. A thorough assessment by a multidisciplinary team, including urologists and oncologists, is essential to determine the best treatment plan.
Robotic VEIL surgery represents a significant advancement in the treatment of penile cancer. By offering a minimally invasive option with numerous benefits, this technique not only improves surgical outcomes but also enhances the overall patient experience. As technology continues to evolve, we can expect even more innovative solutions to emerge in the fight against cancer.
Dr. Rohit Kaushal is a leading Urologist and Robotic Surgeon in Delhi, specializing in kidney transplant, prostate, and reconstructive urology with compassionate patient care.
© 2025 Created with Digital Growth Well